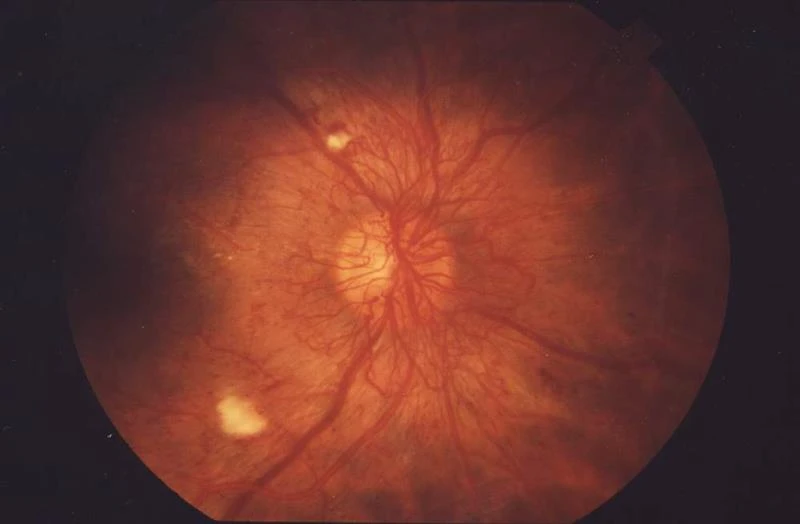
Diabetic Retinopathy: The Silent Threat to Vision Diabetes is one of the most widespread chronic conditions globally—especially in India, where it affects millions across all age groups. But it’s not just high blood sugar levels that are concerning—it’s the serious complications that follow. One of the most dangerous, yet often overlooked, is Diabetic Retinopathy (DR), an eye condition that affects approximately 16.9% of diabetic individuals. Fortunately, with modern eye scanning technology, early detection is now faster, simpler, and more accurate—offering hope and protection against vision loss. What is Diabetic Retinopathy? Diabetic Retinopathy occurs when prolonged high blood sugar damages blood vessels in the retina, the light-sensitive tissue at the back of the eye. Over time, these vessels may leak, swell, or close off. In advanced stages, abnormal new vessels may grow, leading to bleeding, scarring, and potential blindness. Common Symptoms Blurred or fluctuating vision Dark spots or “floaters” Partial or total vision loss in later stages Note: In early stages, there are often no symptoms at all—making regular eye screening essential for anyone with diabetes. How Eye Scanning Helps Detect DR Eye scanning uses non-invasive, high-resolution imaging tools to capture detailed views of the retina, allowing early signs of damage to be spotted—often before you notice any change in vision. 1. Fundus Photography High-definition image of the retina using a specialized camera Detects: Leaky blood vessels Retinal swelling (macular edema) Hemorrhages and microaneurysms Quick and painless; usable in clinics or mobile vans 2. Optical Coherence Tomography (OCT) Cross-sectional images of the retina using light waves Shows: Retinal thickness and swelling Fluid accumulation Excellent for monitoring disease progression 3. AI-Powered Retinal Scanning AI tools analyze retinal scans instantly Benefits: High accuracy Immediate results Remote screening access Some FDA-approved tools allow diagnosis without a specialist Should You Get Screened? According to international guidelines: Type of Diabetes Recommended Screening Time Type 1 Diabetes Within 5 years of diagnosis, then yearly Type 2 Diabetes At the time of diagnosis, then yearly Diabetic Pregnant Women Before pregnancy or during first trimester Tip: Your ophthalmologist may recommend more frequent exams based on your condition. Why Early Detection Matters When caught early, diabetic retinopathy is far more treatable. Early detection allows: Vision loss to be prevented or delayed Effective treatments: laser therapy, injections, or surgery Improved long-term eye health and quality of life A Vision for the Future Thanks to innovations in: Non-invasive imaging Portable scanning devices AI-based diagnostics Diabetic eye care is becoming more accessible, even outside traditional eye clinics. Screenings can now happen in primary care clinics, pharmacies, or community health programs. Note: Technology isn’t a replacement for care. Maintaining blood sugar levels and attending regular eye checkups is key. Final Thought If you or someone you love has diabetes, don’t wait for symptoms. Schedule a comprehensive eye scan Ask your doctor about diabetic retinopathy Spread awareness in your community Your vision matters. Scan early. See clearly. Live fully. Fundus Showing Diabetic Macular Edema (DME) and Capillary Dropout This image highlights hallmark signs of diabetic retinopathy such as fluid leakage and vessel damage near the fovea—ideal for discussing early-stage pathology.

Mammography has long been a critical tool in the early detection of breast cancer and has saved countless lives through timely diagnosis. However, like all medical procedures, it comes with certain limitations and potential risks. As awareness grows, many women are seeking safer, more comfortable alternatives. One promising method on the rise is thermal imaging, also known as thermography. Concerns with Mammography 1. Radiation Exposure Mammography uses low-dose ionizing radiation. While the exposure is minimal, repeated screenings—especially from a younger age—may slightly increase cancer risk. Women with genetic sensitivity to radiation, such as those with ATM gene mutations, should discuss this with their doctor. 2. False Positives and Unnecessary Anxiety A false positive suggests cancer where none exists. Over a 10-year period, over 50% of women screened annually will have at least one false positive. This often leads to unnecessary biopsies, emotional distress, and additional medical procedures. 3. Overdiagnosis and Overtreatment Some detected tumours may be extremely slow-growing or non-lethal. Treating these may expose women to unnecessary interventions like surgery, radiation or chemotherapy—with little health benefit. 4. Discomfort and Pain Mammography requires breast compression, which many find uncomfortable or painful. This discomfort may deter women from regular screenings, especially those with sensitive tissue or past trauma. 5. False Negatives Mammograms can miss cancers, especially in women with dense breast tissue—common in younger women. This gives a false sense of security and may delay treatment. What Is Thermal Imaging? Thermal imaging (thermography) is a non-invasive, radiation-free technique that uses infrared cameras to detect heat patterns and blood flow in tissues. Cancerous cells tend to produce more heat due to rapid growth and increased blood supply, making this an innovative way to spot abnormalities before a tumour even forms. Thermal Imaging vs. Mammography: A Comparison Feature Mammography Thermal Imaging (Thermography) Radiation Yes (low-dose ionizing radiation) No radiation Contact and Discomfort Requires breast compression No contact or compression Type of Detection Structural changes (tumours, masses) Physiological changes (heat, vascularity) Accuracy in Dense Breasts Lower accuracy, risk of false negatives More reliable for dense tissue Risk of False Positives/Negatives High in some cases Lower in some cases (technology evolving) Screening Frequency Every 1–2 years Can be done more frequently and safely Advantages of Thermal Imaging Radiation-Free: Safe for all ages, including younger women and those needing more frequent monitoring. Comfortable and Painless: No compression, no discomfort—just a quick and non-invasive scan. Early Detection of Physiological Changes: Can detect signs like inflammation or abnormal blood flow years before a tumour becomes detectable by other means. Ideal for Dense Breast Tissue: Provides better results for women whose breast density reduces the accuracy of mammograms. Frequent Monitoring Possible: Because it’s safe and non-invasive, it’s ideal for high-risk women, those with family history, or those undergoing hormone therapy. Making an Informed Choice This article is not a critique of mammography—but a call for personalised, informed decision-making. Mammography remains invaluable, especially for women over 50 or those at higher risk. But if you’re looking for a radiation-free, painless, and more frequent screening option, thermal imaging is a powerful complement—or even alternative. Always consult your doctor to choose the screening strategy best suited to your age, health and risk factors.

What Every Woman Should Know Just hearing the words, Breast Cancer, can bring a wave of anxiety to a woman. Yes, Breast cancer is one of the most common cancers in women today, especially in metro cities. But here’s the hopeful truth—when detected early, breast cancer is highly treatable and the chances of survival are significantly higher. Early detection doesn’t just save lives—it improves the quality of those lives by making treatment less aggressive and more effective. So, here’s what you need to know about breast cancer and how to catch it early. What Is Breast Cancer? Breast cancer occurs when cells in the breast grow uncontrollably, forming a tumour that can be felt as a lump or seen on medical imaging. Though it primarily affects women, men can also develop breast cancer. It is one of the most common cancers among women globally especially due to our modern lifestyle. Why Early Detection Matters Early detection can: Increase the chances of successful treatment. Allow for less aggressive treatment options. Lower the risk of cancer spreading to other parts of the body. Reduce treatment costs and emotional stress. In fact, when breast cancer is found early—before it has spread beyond the breast—the 5-year survival rate is about 99%. Key Methods of Early Detection 1. Breast Self-Examination (BSE) It involves becoming familiar with the look and feel of your breasts and helps you notice changes early. Perform it monthly, ideally a few days after your menstrual cycle ends. Look for lumps, dimpling, nipple discharge or changes in size/shape. 2. Clinical Breast Exam Conducted by a doctor or nurse during routine check-ups. Helps catch anything that might not be obvious during self-exams. 3. Mammography It’s a low-dose X-ray of the breast that can detect tumours before they can be felt. Recommended every 1–2 years for women over 40 or earlier for those with higher risk. Breast compression can be painful or uncomfortable, discouraging some women from regular screening. Mammograms may detect something suspicious that turns out to be non-cancerous. 4. Thermal Imaging / Thermography It is a non-invasive, radiation-free technique that uses infrared cameras to detect heat patterns and blood flow in body tissues. Since cancer cells tend to grow rapidly and generate more heat than normal tissues, thermography can detect abnormal activity before a tumour forms. 5. Ultrasound and MRI These are not primary diagnostic tools but supplementary tools. They are especially helpful for women with dense breast tissue or high genetic risk. Know Your Risk Factors Some risk factors are beyond your control, but knowing them helps guide decisions: Age: Risk increases with age. Family History: A mother, sister or daughter with breast cancer raises your risk. Genetics: BRCA1 and BRCA2 gene mutations can significantly increase risk. Hormone Exposure: Early menstruation, late menopause and hormone therapy can raise risk. Lifestyle: Smoking, excessive alcohol, poor diet and lack of exercise are lifestyle-related risks. What You Can Do Today Schedule regular check-ups Talk to your doctor about your personal risk Adopt a healthy lifestyle Learn and practice breast self-exams Share awareness with other women Breast cancer doesn’t have to be feared. Awareness, vigilance and action can turn fear into empowerment. Early detection doesn’t just save lives—it gives women more years of health, laughter, happiness and life.

Diabetes is a growing global health crisis—and with India often referred to as the “diabetes capital of the world”, millions are affected. While many understand the toll diabetes takes on blood sugar and overall health, fewer are aware of a serious and often silent complication: Diabetic Retinopathy, a condition that can irreversibly damage vision. What Is Diabetic Retinopathy? Diabetic Retinopathy is an eye condition that affects individuals with diabetes. It occurs when high blood sugar levels damage the tiny blood vessels in the retina—the light-sensitive tissue at the back of the eye. Over time, these vessels may leak, swell, or close off completely, leading to vision impairment or even blindness. Stages of Diabetic Retinopathy This condition progresses gradually, often without noticeable symptoms in its early stages. The four main stages are: 1. Mild Non-Proliferative Retinopathy Small balloon-like swellings called microaneurysms develop in the retinal blood vessels. 2. Moderate Non-Proliferative Retinopathy Some blood vessels that nourish the retina become blocked, reducing oxygen supply. 3. Severe Non-Proliferative Retinopathy A larger number of vessels are blocked, prompting the retina to signal for the growth of new blood vessels. 4. Proliferative Diabetic Retinopathy (PDR) The most advanced stage, where abnormal and fragile new blood vessels form on the retina and in the vitreous (the gel-like fluid inside the eye). This can lead to bleeding, retinal detachment, and permanent vision loss. Warning Signs to Watch For Diabetic Retinopathy often advances silently. Regular eye exams are crucial because symptoms typically appear only in later stages. Be alert to the following signs: Blurred or fluctuating vision Dark spots or “floaters” Impaired color perception Partial or total vision loss If you experience any of these symptoms—especially if you are diabetic—see an eye specialist without delay. Who’s at Risk? Anyone with diabetes—Type 1, Type 2, or gestational—can develop diabetic retinopathy. The risk increases due to: Poorly controlled blood sugar levels High blood pressure Elevated cholesterol Long-standing diabetes (duration matters) Smoking Pregnancy in women with pre-existing diabetes Take Control: Prevention and Management The good news is that diabetic retinopathy is preventable and manageable if caught early. Here’s what you can do: Get regular dilated eye exams—at least once a year Control your blood sugar, blood pressure, and cholesterol levels Avoid smoking and limit alcohol Maintain a healthy lifestyle with balanced nutrition and exercise Consult your doctor immediately if you notice any vision changes Final Thoughts: Don’t Let Diabetes Take Your Sight Diabetic Retinopathy may not show early symptoms, but that doesn’t mean it’s harmless. With timely screening, good diabetes management, and access to appropriate treatment, most cases of vision loss can be prevented. Have you had your eyes checked this year? Don’t wait—your sight is too precious to lose.
India often celebrates topping global charts—but being called the “diabetic capital of the world” is no badge of honor. With over 77 million diagnosed diabetic patients and 25 million more pre-diabetic individuals, diabetes has reached near-endemic levels in the country. Indians are more genetically and culturally predisposed to Type 2 diabetes than many other populations. This increased vulnerability stems from a mix of genetic, lifestyle, and environmental factors. Despite its growing prevalence, many people still ask: “What exactly is diabetes?”, “Why does it happen?”, or “Can it be prevented?” This article aims to answer those questions simply and clearly—because when it comes to health, knowledge is power. What Is Diabetes? Diabetes mellitus is a chronic condition in which the body cannot properly regulate blood sugar (glucose) levels. Glucose is the main energy source for our body and comes from the food we eat. To process glucose, our body uses insulin, a hormone produced by the pancreas. In diabetes, this process is disrupted—either due to insufficient insulin production or the body’s inability to use insulin effectively. Types of Diabetes Type 1 Diabetes Cause: An autoimmune condition that destroys insulin-producing cells in the pancreas. Onset: Typically in childhood or adolescence. Management: Daily insulin injections or use of an insulin pump. Type 2 Diabetes Cause: The body becomes resistant to insulin or doesn’t produce enough of it. Onset: Most common in adults but increasingly seen in younger individuals due to poor lifestyle habits. Management: Lifestyle changes, oral medications, and sometimes insulin therapy. Gestational Diabetes Cause: Develops during pregnancy in women without a prior diabetes diagnosis. Risks: Increases chances of complications during pregnancy and developing Type 2 diabetes later in life. Prediabetes Definition: Blood sugar levels are elevated but not high enough for a Type 2 diagnosis. Importance: A critical warning sign that offers a chance for prevention through lifestyle changes. Symptoms of Diabetes While some individuals show symptoms early, others may remain undiagnosed until complications occur. Common signs include: Frequent urination Excessive thirst or hunger Fatigue Blurred vision Slow healing wounds Numbness or tingling in hands and feet Sudden weight loss (more common in Type 1) Complications of Uncontrolled Diabetes Unchecked diabetes can damage almost every organ in the body. Major complications include: Cardiovascular issues: Heart disease and stroke Kidney damage: Diabetic nephropathy Eye conditions: Diabetic retinopathy, glaucoma, cataracts Nerve damage: Neuropathy Foot problems: Infections, ulcers, amputations How Is Diabetes Diagnosed? Doctors use several tests for diagnosis: Test Purpose Fasting Blood Sugar Test Measures blood sugar after overnight fasting HbA1c Test Shows average blood sugar over 2–3 months Oral Glucose Tolerance Test Measures how your body processes glucose Random Blood Sugar Test Checks sugar levels regardless of last meal time The New-Age Early Detection: Eye Screening In addition to traditional tests, eye screening is emerging as a powerful early detection tool. Diabetes can silently damage your eyes, often without early symptoms. That’s where fundus photography, enhanced with Artificial Intelligence (AI), comes in. This advanced technology captures high-resolution images of the back of the eye, allowing early diagnosis without the discomfort of traditional dilation drops. Early detection through eye scans can prevent blindness and flag the onset of diabetes-related complications. Final Thoughts: Take Control Today Diabetes doesn’t have to define your life. By being proactive, making healthy choices, and staying informed, you can prevent or manage the condition effectively. Get regular screenings Maintain a healthy diet and weight Stay physically active Understand your genetic risk Keep an eye on your eye health Your health is in your hands. Act today, live better tomorrow.

When you’re young, aging feels like a distant reality. But once you cross that milestone of 50, the question hits: “How do I stay healthy, active, and independent as I grow older?” Aging is inevitable—but how you age is up to you. That’s the heart of Healthy Aging—not just avoiding illness, but nurturing your physical, mental, and emotional well-being so you can enjoy life to the fullest. What Is Healthy Aging? Healthy aging means more than just living longer—it means living better. It’s about maintaining independence, vitality, and happiness as the years go by. Healthy aging involves adopting habits that minimize the risk of disease, disability, and frailty, while maximizing joy, resilience, and purpose. We like to call this Positive Aging—and yes, it’s absolutely achievable! 6 Key Pillars of Happy & Healthy Aging 1. Physical Activity Regular movement keeps your body strong and your spirits high. Activities like walking, swimming, yoga, or dancing: Improve heart health Help maintain a healthy weight Reduce the risk of chronic illnesses like diabetes, osteoporosis, and hypertension Tip: Choose exercises you enjoy—it’s easier to stick with them long-term. 2. Nutrition Fuel your body with wholesome foods that support energy and immunity: Eat a colorful variety of fruits and vegetables Choose whole grains, lean proteins, and healthy fats Stay hydrated and limit processed foods Good nutrition helps prevent chronic diseases and supports both physical and brain health. 3. Cognitive Stimulation Just like your body, your brain needs regular workouts too. Stimulate your mind by: Reading books or listening to podcasts Learning new skills or hobbies Playing puzzles, memory games, or strategy-based activities Keeping your brain active helps maintain cognitive function and reduces the risk of dementia. 4. Social Engagement Staying connected is key to mental and emotional health. Make time for: Family and friends Community events or local clubs Volunteer work or social support groups Social interaction combats loneliness and enhances your sense of belonging and purpose. 5. Mental & Emotional Well-being Emotional health is just as important as physical health. Prioritize your mental wellness by: Practicing mindfulness or meditation Managing stress through journaling or counseling Seeking support when needed—don’t hesitate to talk to a therapist or loved one Emotional balance boosts resilience and helps you handle life’s ups and downs gracefully. 6. Regular Health Check-Ups Routine medical screenings are essential to catch issues before they become serious. Keep up with: Annual physical exams Blood sugar, cholesterol, and blood pressure checks Eye, dental, and bone density tests Age-specific screenings (e.g., mammograms, colonoscopies) Prevention and early intervention go a long way in preserving health and independence. Final Thought Aging doesn’t have to be something you fear—it can be something you celebrate. With a few mindful choices and consistent habits, you can enjoy a long, fulfilling life full of joy, connection, and purpose.